
Candida auris Cases are on the Rise in Virginia
May 7, 2021
Dear Colleague:
Key Messages
- The Virginia Department of Health (VDH) is reporting a statistically significant increase in Candida auris (C. auris) cases over the past 10 months in multiple regions of Virginia and in multiple types of healthcare facilities. Between September 2018 and June 2020, only three cases of C. auris were identified in Virginia. Since the beginning of July 2020, 37 cases have been identified (Figure 1).
- C. auris is an emerging fungus that is often resistant to antifungal drugs used to treat Candida infections and is difficult to identify with standard laboratory methods.
- All healthcare professionals, inpatient and outpatient, should take measures to prevent the spread of C. auris as recommended in the VDH August 2019 Clinician Letter.
- Patients at highest risk for C. auris colonization are those who reside in or who have had prolonged admissions to high-risk healthcare facilities (particularly long-term acute care hospitals or ventilator skilled nursing facilities) or have had recent international healthcare exposure.
Situation
C. auris is an emerging fungus that presents a serious global health threat. It is often resistant to antifungal drugs used to treat Candida infections, is difficult to identify with standard laboratory methods, and can cause outbreaks in healthcare settings that have resulted in high mortality rates.
VDH is seeing a substantial increase in the number of new C. auris cases in healthcare facilities in Virginia (Figure 1). Surrounding jurisdictions, including Maryland, Pennsylvania, and the District of Columbia, are also experiencing increases in cases. Multidrug resistant organisms (MDRO) such as C. auris or carbapenem-resistant Enterobacteriaceae (CRE) may be spreading due to personal protective equipment (PPE) conservation strategies and other COVID-19 containment practices, particularly in long-term care facilities. Containment of MDROs among patients and residents is critical during the COVID-19 response to prevent concurrent outbreaks and additional spread across the Commonwealth.
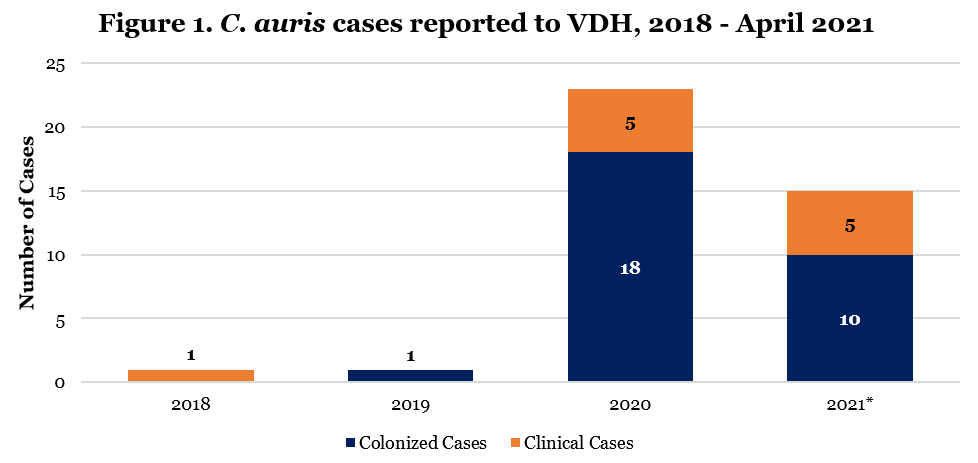
*Data reported to VDH as of May 3, 2021
Actions Requested
Infection Prevention and Control
- Cohort patients by MDRO status and COVID-19 status.
- Do not reuse gloves and gowns between patients with different (or unknown) MDRO and COVID-19 status.
- Place all suspected or confirmed C. auris cases on contact precautions. The same infection control precautions are recommended for patients with C. auris infection and colonization. See CDC’s C. auris Infection Prevention and Control Measures.
- Use an Environmental Protection Agency (EPA)-registered hospital-grade disinfectant effective against C. auris (List K or EPA-claim) to disinfect the rooms of and any shared equipment used by confirmed, presumptive, or suspect C. auris-positive residents.
- Consider doing this universally in facilities with patients with or at high-risk for C. auris and in units of confirmed or high-risk patients.
- Examples of high-risk patients include patients with tracheostomies, those who are ventilator dependent, those colonized with other MDROs, or those who have recently received antibiotics or antifungals
- Continue to implement other MDRO containment practices including:
- Perform hand hygiene before putting on PPE, after removing PPE, before and after patient contact, and after contact with the patient’s immediate surroundings.
- Perform routine cleaning and disinfection of surfaces and shared medical equipment with an EPA-registered hospital-grade disinfectant effective against C. auris (List K or EPA-claim), COVID-19 (List N), and/or other pathogens according to the manufacturer’s instructions.
- Use checklists to identify who is responsible for cleaning each item and cleaning frequency (e.g. environmental services staff versus clinical staff).
- Educate staff on the appropriate infection prevention and control practices and the application of safety sciences.
- Consider doing this universally in facilities with patients with or at high-risk for C. auris and in units of confirmed or high-risk patients.
Communication
- Communicate a patient’s MDRO status to any receiving healthcare facility. This is especially important so that patients with MDROs can be placed on appropriate precautions.
- Obtain patient history about any recent international healthcare exposure, exposure to C. auris, prior MDRO status, or stays in a healthcare facility with known transmission of C. auris.
- Screen patients at high risk for C. auris. Place high risk patients on empiric contact precautions while test results are pending.
- If you need assistance determining screening criteria for high-risk or potentially exposed patients for C. auris, please contact VDH at hai@vdh.virginia.gov for assistance.
- Report all suspected and confirmed C. auris cases to your local health department per the Virginia Reportable Disease List.
Testing
- C. auris can be misidentified as a number of other organisms when using traditional biochemical methods for yeast identification. Labs should review the CDC’s Identification of Candida auris recommendations. Therefore, it is important to confirm that your laboratory can detect C. auris or presumptive C. auris.
- As a provider, it is also important to recognize the importance of C. auris upon receipt of a lab report so that it is not inadvertently confused with other Candida species. Speciation of Candida from non-sterile sites is not usually performed, so clinicians should request their laboratory to identify the species of Candida isolates obtained from both sterile and non-sterile sites, particularly for patients at high risk for C. auris:
- Patients admitted to facilities where a case of C. auris colonization or infection has been detected
- Patients currently or recently residing in skilled nursing facilities with ventilated patients or in long-term acute care hospitals
- Patients with an overnight stay in a healthcare facility outside the U.S. in the previous year, especially in a country with documented C. auris transmission.
Resources
- CDC C. auris website: https://www.cdc.gov/fungal/candida-auris/health-professionals.html
- VDH C. auris website: https://www.vdh.virginia.gov/haiar/diseases-organisms/candida-auris/
Thank you for your continued efforts to protect Virginians from multidrug resistant organisms, particularly in the context of the COVID-19 pandemic.
Sincerely,
M. Norman Oliver, MD, MA
State Health Commissioner
