VIPTA is a statewide infection prevention and control education collaborative, led by the Virginia Healthcare-Associated Infections Advisory Group. Through partnership, VIPTA curates IPC resources for Virginia’s healthcare, congregate care, and public health settings.
Upcoming Events
It’s Not Just a Room Turnover: It’s Infection Prevention
Did you know that patients admitted to rooms where the previous occupant had a multidrug-resistant organism (MDRO) face a higher risk of acquiring that same organism? Every day, environmental services (EVS) professionals work alongside frontline healthcare staff to reduce this risk and protect patients and residents. When we support EVS teams, we strengthen the entire infection prevention system.
What to Expect and How to Use It: With some EVS staff receiving as little as three days of training, and 83% learning on the job, education needs to be quick, practical, and built into their daily workflow.
- Onboarding: Project Firstline Training Toolkit for Environmental Services (EVS) Staff – A comprehensive training plan that builds both the why and the how, helping EVS staff confidently step into their role as essential infection prevention team members.
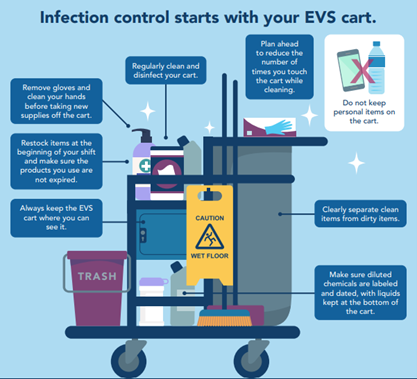
- New Refreshers: CDC EVS Microlearns – Quick, practical micro-learns covering key topics like contact time, when to change gloves, and maintaining clean and safe EVS carts, perfect for reinforcing skills in just a few minutes.
- New Observation & Support: VDH Daily Room Cleaning Checklist – A simple, structured checklist to guide room cleaning from start to finish, helping standardize workflows and ensure no critical steps are missed.
Target Audience: Essential IPC Education Level
Guidance & Regulation Updates
VIPTA members track guidance and regulation resources to share source documents that guide infection prevention and control practices for public health staff and clinical and non-clinical healthcare personnel.
The date of the regulation or guidance update is included in each post. Please check linked content to be sure it is the most up to date and recommended practice.
CDC: Considerations for Reducing Risk – Water in Healthcare Facilities (2/6/2026)
ASHRAE: Ventilation of Healthcare Facilities (2/16/2026)
CDC: Updated 2026 National Healthcare Safety Network (NHSN) Surveillance Protocols (January 2026)
APIC: New White Paper on Centralized Health-Associated Infection Surveillance Programs and Micro-Credential to Advance Centralized HAI Surveillance and Patient Safety (1/20/2026)
VDH: Clinician Letter: Respiratory Illness and Measles Updates for Virginia (1/21/2026)
✨Innovative Antimicrobial Stewardship Education in Long-Term Care: A Virginia Beach Success Story
Whitney Rice, MPH, CIC, Healthcare-Associated Infections Epidemiologist at the Virginia Beach Department of Public Health, has taken a proactive and creative approach to antimicrobial stewardship in long-term care settings. Inspired by a successful initiative from another Virginia health district, Rice launched an educational campaign across three types of long-term care facilities: skilled nursing facilities, assisted living facilities (ALFs), and multicare centers.
The program was designed to reach all key stakeholders (e.g., providers, residents, and families) with tailored educational materials and interactive sessions. These included PowerPoint presentations, printed handouts, activity books, and engaging games such as a microbe matching challenge (to distinguish between bacterial and viral infections) and a Jeopardy-style quiz game for staff. A post-education survey revealed overwhelmingly positive feedback: residents enjoyed the sessions, and staff expressed interest in more in-depth technical content.
Key Educational Messages:
- For Residents and Families: Emphasis was placed on the importance of taking antibiotics exactly as prescribed, on time and without skipping doses, and understanding that antibiotics are ineffective against viral infections.
- For Providers: The training focused on resisting pressure to prescribe unnecessary antibiotics and included guidance on managing multidrug-resistant organisms (MDROs), with a focus on cleaning, disinfection, and Enhanced Barrier Precautions to prevent their spread.
Lessons Learned:
- Skilled Nursing Facilities: These settings yielded the most effective provider education, likely due to the more consistent presence of medical staff and pharmacists.
- Assisted Living Facilities: Provider education was more challenging here due to fewer on-site clinicians, but resident engagement was highest, as ALF residents were more able to actively participate in the sessions.
- Future Plans: These insights will be used to refine and tailor future rounds of education, ensuring that content delivery is optimized for each facility type and audience.
Whitney Rice’s initiative demonstrates how thoughtful, audience-specific education can enhance antimicrobial stewardship and promote responsible antibiotic use in long-term care environments. Her work serves as a model for those seeking to make a meaningful impact in their communities.
IPC Education & Training Library
Search the VIPTA library of curated infection prevention and control (IPC) education and training resources. The IPC Education & Training Resource Library includes state and national resources related to healthcare-associated infections, antimicrobial resistance and/or IPC. Visit the VIPTA FAQ page to learn more about VIPTA library content.